This is the email I wish every doctor in India would send their patients.
Because here’s a number that should terrify you:
38.6% of Indian adults have non-alcoholic fatty liver disease.
That’s 1 in 3. And most of them have no idea.
No symptoms. No pain. Just a liver that’s slowly drowning in fat while you go about your day thinking everything is fine because your “routine blood work came back normal.”
Why Your Doctor Probably Missed It
Standard blood tests check your ALT and AST (liver enzymes). But here’s the problem: fatty liver can exist with completely normal ALT levels. A 2023 study in the Journal of Hepatology found that up to 50% of people with significant liver fat had normal liver enzyme readings.
The only way to catch it early? An ultrasound. And most doctors don’t order one unless you’re already showing symptoms.
By then, you’re often at Grade 2 or Grade 3.
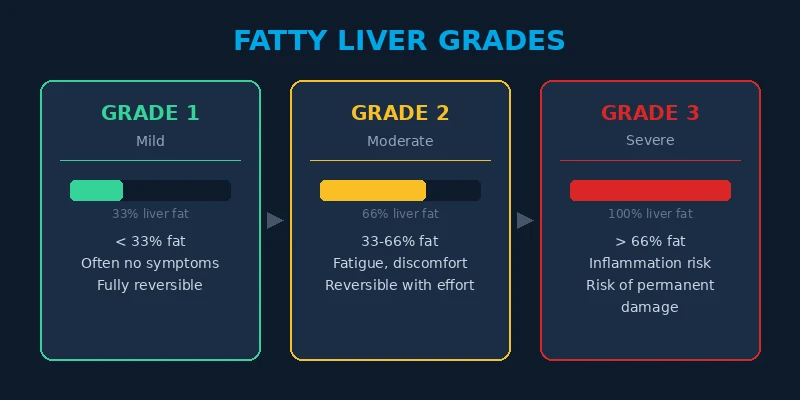
The 3 Things That Cause Fatty Liver (It’s Not Alcohol)
When I say “fatty liver,” most people think alcohol. But non-alcoholic fatty liver disease (NAFLD) is now the most common liver disease in India, and it has nothing to do with drinking.
The three drivers:
- Excess refined carbs after 6 PM. Your liver converts unused carbohydrates into fat. When you eat most of your carbs at dinner (which 80% of Indian professionals do), your liver gets flooded with sugar right when your metabolism is at its slowest.
- Fructose overload. Not from fruit — from packaged juices, biscuits, sauces, and “health drinks.” Fructose is processed exclusively by your liver. Too much of it = direct fat deposit.
- Visceral fat. The belly fat you can’t pinch. Even people at “normal” weight can have dangerous visceral fat wrapping around their liver. In India, this is called “thin on the outside, fat on the inside” — and it’s incredibly common in IT professionals who sit 10+ hours a day.
“My Ultrasound Said Grade 2. My Doctor Said Lose Weight. That Was It.”
I hear this story every single week.
A client comes to me with an ultrasound showing Grade 2 fatty liver. Their doctor said “lose weight and avoid oily food.” No plan. No structure. No follow-up.
So they do what everyone does: they Google “fatty liver diet plan” and find a list of foods to avoid. They cut oil completely. They stop eating rice. They start drinking warm lemon water every morning.
Three months later, nothing has changed. Because the problem was never “oily food.”
What Actually Reverses Fatty Liver
A 2025 study published in ScienceDirect followed NAFLD patients through sustained lifestyle intervention. The results:
- 85.2% achieved weight reduction
- 40.5% had a one-stage fibrosis regression
- 52% showed a 2-point reduction in liver stiffness
The intervention wasn’t a juice cleanse. It wasn’t a detox. It was structured eating patterns combined with progressive activity. The same approach we use at THINQ.FIT.
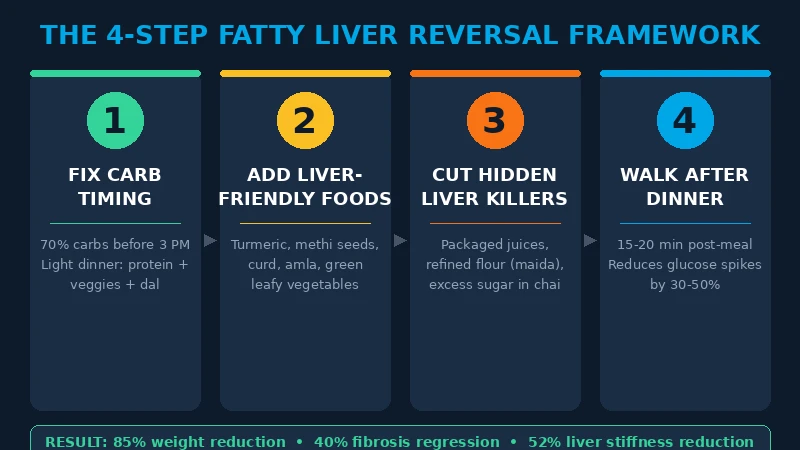
The THINQ.FIT Fatty Liver Framework
Here’s exactly what we do with fatty liver clients. No supplements. No expensive foods. Just restructuring what you already eat.
Step 1: Fix the Carb Timing
Move 70% of your carbohydrates (rice, roti, bread) to before 3 PM. This gives your liver time to process them when insulin sensitivity is at its peak. At dinner, focus on protein + vegetables + a small portion of dal.
This single change reduces the overnight fat deposit in your liver by a significant margin.
Step 2: Add These 5 Liver-Friendly Indian Foods
You don’t need imported superfoods. These are in every Indian kitchen:
- Haldi (Turmeric) — curcumin reduces liver inflammation. Use it in dal, sabzi, and milk. Not supplements. Real turmeric, with black pepper for absorption.
- Methi (Fenugreek) seeds — soak 1 tablespoon overnight, drink the water on an empty stomach. Reduces liver fat and improves insulin sensitivity.
- Curd/Dahi — probiotics support gut-liver axis health. A 2024 review in Frontiers in Microbiology confirmed that gut microbiota plays a direct role in NAFLD progression.
- Amla (Indian Gooseberry) — one of the richest sources of Vitamin C. Protects liver cells from oxidative damage.
- Green leafy vegetables — palak, methi leaves, amaranth. The nitrates help reduce liver fat. Aim for one serving at lunch and one at dinner.
Step 3: Cut These 3 Hidden Liver Killers
- Packaged fruit juices — even “100% natural” juices are fructose bombs. Eat the whole fruit instead.
- Refined flour (maida) — naan, white bread, biscuits, bakery items. Switch to whole wheat or millets.
- Sugar in chai — 4 cups of chai with 2 spoons of sugar each = 32 grams of added sugar daily. Your liver processes every gram.
Step 4: Walk After Dinner
A 15-20 minute walk after your last meal does something remarkable: it activates your muscles to absorb glucose directly from your bloodstream, bypassing your liver entirely. This reduces the load on your liver at the time it needs relief the most.
Research shows that post-meal walking reduces blood glucose spikes by 30-50%. For fatty liver patients, this is one of the highest-impact habits you can build.
What You Can Do This Week
You don’t need a coach to start. Try this for 7 days:
- Shift your largest rice/roti portion to lunch. Dinner should be your lightest meal.
- Add turmeric to one dish daily. With a pinch of black pepper.
- Replace packaged juice with whole fruit. One orange > one glass of “fresh” orange juice.
- Walk 15 minutes after dinner. Not a workout. Just a walk.
- Get an ultrasound. If you haven’t had one in the last year and you carry weight around your belly, ask your doctor for a liver ultrasound. It costs ₹800-1500 and takes 10 minutes.
If your ultrasound shows Grade 1, these changes alone can reverse it within 3-6 months.
If it shows Grade 2 or higher, you need a structured plan — not a diet chart from Google. That’s where coaching makes the difference.
Next week: PCOD and weight loss — why the standard “eat less, exercise more” advice fails every woman with polycystic ovaries, and what actually works.


